Published Research in Nature Identifies Five Genetic Factors That Connect Depression, Anxiety, Schizophrenia, ADHD, and Other Mental Disorders.
A global study found that 14 psychiatric disorders share five common genetic roots, indicating that genetic factors explain much of the biological similarity between these conditions, according to research published in December 2025 in the journal Nature.
The international team, led by scientists from the United States and Europe, analyzed genetic data from over 1 million people diagnosed with at least one psychiatric disorder and 5 million without a diagnosis, allowing them to map common patterns in DNA.
The result, obtained in the United States and through various partner institutions, suggests a path to understanding why many patients have more than one diagnosis throughout their lives and may influence future treatments.
-
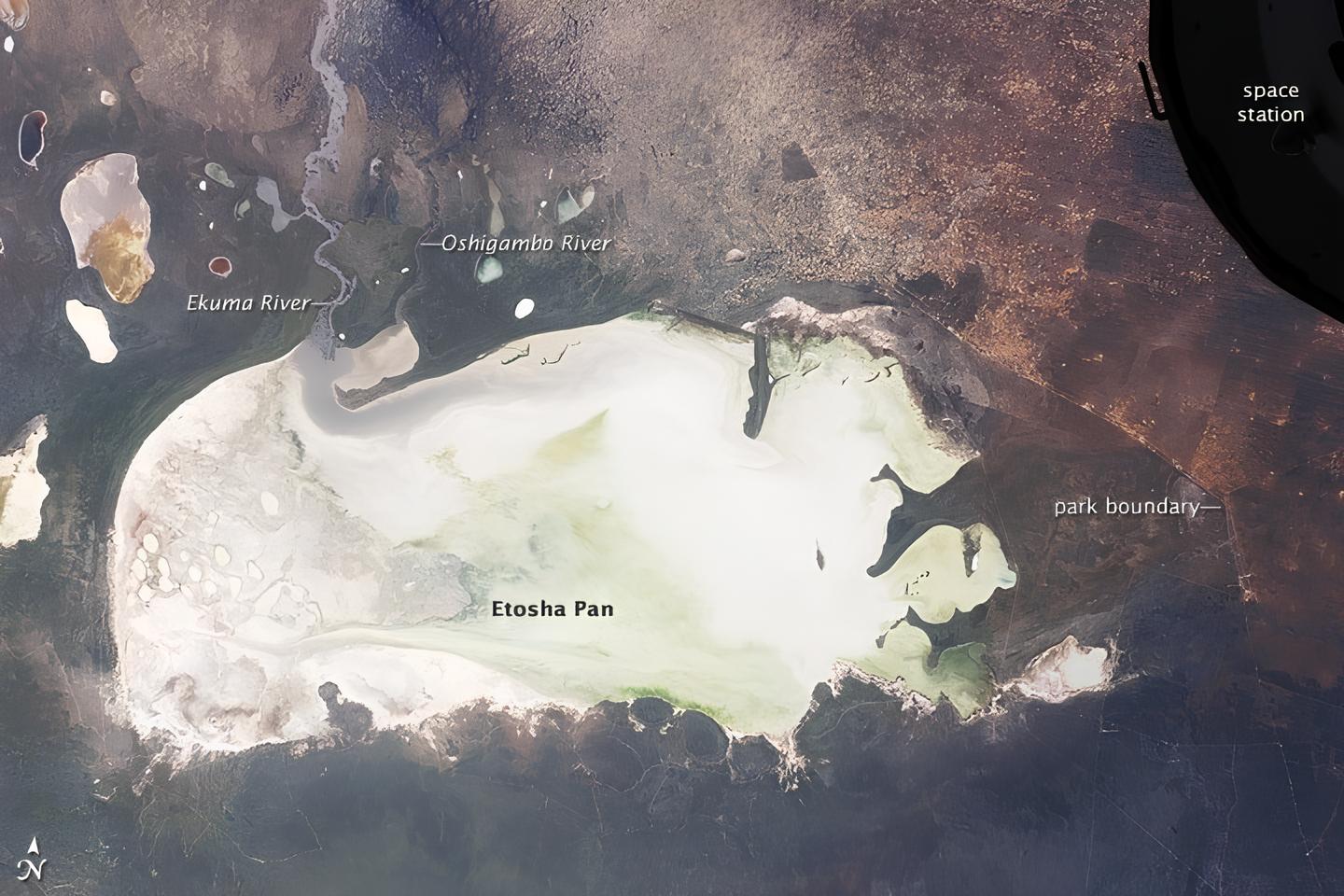
A lake in Antarctica hides water with rare chemistry, a depth of nearly 170 meters, and microbial structures that help scientists search for signs of life on Mars.

-
Elon Musk is trying to transform Starlink into the new standard for in-flight Wi-Fi, and the orbital war between giants is changing the sky of commercial aviation.

-
Collapse in sight in Iraq: satellite images captured by NASA show the country’s largest reservoir dramatically drying up.
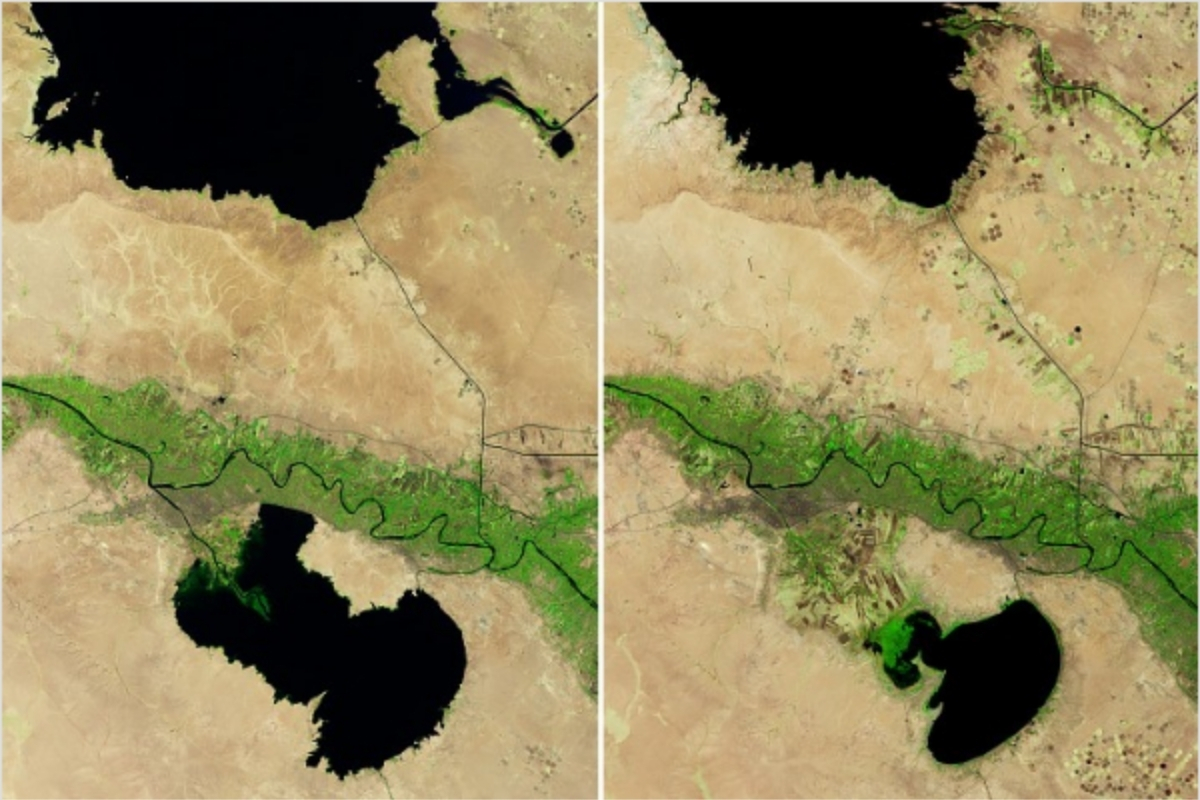
-
Archaeologists open a tomb in Luxor and find 3,000-year-old papyri still sealed in a ceramic vessel, alongside colorful coffins stacked in 10 rows and linked to the mysterious singers of Amon.

Genetics and Psychiatric Disorders: Five Shared Factors
The detailed analysis revealed that the 14 psychiatric disorders studied are not as genetically distinct as they were thought to be.
Instead, the research identified five main genetic factors that influence most conditions, composed of 238 distinct genetic variants.
Each of the five groups summarized a set of shared genetic characteristics among various conditions:
- Disorders with Compulsive Traits, such as obsessive-compulsive disorder (OCD) and anorexia nervosa.
- Internal Conditions, including depression, anxiety, and post-traumatic stress disorder.
- Substance Use Disorders, such as alcohol or other drug dependence.
- Neurodevelopmental Conditions, such as autism and ADHD (attention deficit hyperactivity disorder).
- Severe Psychiatric Disorders, such as schizophrenia and bipolar disorder, which share approximately 70% of genetic signals.
This grouping shows that genetics can explain why these disorders often occur together or have overlapping symptoms, a phenomenon observed in clinical practice for a long time.
Why This Discovery in Genetics Matters?
For decades, psychiatrists have diagnosed individuals based on the symptoms they present, often without clear biological confirmation.
This explains why a patient with a psychiatric disorder often receives an additional diagnosis of another condition over time — such as anxiety alongside depression, for example.
The new genetic analysis suggests that these conditions are not completely separate entities, but share fundamental biological components.
Thus, genetics may be the key to understanding why a patient with one disorder is more likely to develop another.
How The Study Was Conducted
The researchers from the so-called Psychiatric Genomics Consortium (PGC) collected and analyzed DNA data from millions of participants, including over 1 million with at least one diagnosis of a psychiatric disorder and another 5 million without a diagnosis.
They compared genetic variants between these groups to identify patterns that occur more frequently in individuals with disorders.
Using advanced genetic analysis techniques — which examine small variations in DNA code — the scientists were able to identify common patterns that repeat across different psychiatric conditions.
These methodologies are based on large global databases and statistical models that can separate genetic signals from random noise.

Interpretation of Results and Limitations
Despite the significant advancement, researchers warn that genetics alone does not determine the emergence of psychiatric disorders.
Environmental factors, life experiences, and complex interactions between genes and the environment also influence when, how, and if a disorder manifests.
Moreover, although the study reveals common genetic roots, it does not replace current clinical diagnoses based on observed symptoms and behaviors.
Still, understanding the genetic bases can help create more effective treatments that do not rely solely on superficial symptoms, but on underlying biological processes.
What Could Change in Medical Practice?
Based on these data, experts hope that in the future psychiatric medicine may:
- Redefine how psychiatric disorders are classified, focusing on biological causes rather than isolated symptoms.
- Enhance treatment strategies, potentially developing therapies that target shared genetic mechanisms.
- Better predict comorbidity risk, or the likelihood of a patient developing multiple disorders over their lifetime.
These prospects are not immediate but indicate a paradigm shift: understanding the influence of genetics on psychiatric disorders could open new avenues for personalized interventions.
The authors of the study state that future research should expand to even more diverse populations and include more genetic data. This will allow for refining the understanding of how genetics interacts with social, cultural, and environmental factors to shape mental health.

 Portuguese
Portuguese  English
English  Spanish
Spanish 




-

-

-

-

-

17 pessoas reagiram a isso.