Silent and recurrent infection, simple herpes circulates widely among Brazilian adults, remains in the body for life, and can reappear at different times, even without continuous symptoms. Easy transmission, low initial perception, and risk of reactivation help explain its wide dissemination.
Simple herpes is a widely spread viral infection with easy transmission, with high circulation in Brazil and worldwide.
The Brazilian Society of Dermatology reports that more than 90% of the Brazilian adult population has come into contact with the virus at some point, while the Ministry of Health highlights that only a portion of those infected develop noticeable symptoms.
Even when the lesions disappear, the body does not eliminate the infectious agent, which remains in a latent state and can reappear throughout life.
-
The São Paulo city has one doctor for every 100 inhabitants and still holds the title of the third best place to live in Brazil.

-
Brazilian chocolate made with fine cocoa from Bahia, without any preservatives or chemical additives, won second place for the best milk chocolate in the world and is now sold in the country that invented premium chocolate: Switzerland.

-
For less than 41 thousand reais, you can get a ready-to-move-in studio made from a shipping container with a balcony, a complete bathroom, a kitchen, and total customization of doors, floors, and colors. The most surprising thing is that it all starts from a refrigerated container.

-
A cold air mass that will bring autumn already has a date to arrive and promises to drop temperatures from up to 37°C to a minimum of 10°C, after a sequence of 9 days above 30°C and extreme heat out of the ordinary.
The infection is caused by the Herpes simplex virus, known by the acronym HSV, and is divided into two main types.
In general, HSV-1 is more associated with lesions in the mouth, lips, and nearby areas, although it can also affect the genital region.
On the other hand, HSV-2 is usually related to genital herpes, primarily transmitted through sexual contact, although both types can cause sores in different parts of the body.
In practice, the wide dissemination of herpes helps explain why so many people live with the virus without knowing.
The World Health Organization estimates that most HSV infections go unnoticed or present mild signs, which favors silent transmission.

In many cases, contact occurs in childhood, in the case of HSV-1, or throughout sexual life, in the case of HSV-2, without the person immediately realizing the infection.
How simple herpes acts in the body
Once it enters the body, herpes settles in nerve cells and alternates between periods of inactivity and reactivation phases.
This is why the temporary absence of symptoms does not mean cure.
The virus can remain dormant for long intervals and reappear to cause lesions when it encounters favorable conditions, such as episodes of fever, emotional stress, intense sun exposure, hormonal changes, local injuries, or situations that compromise the immune response.
When there is clinical manifestation, the most common signs include burning, itching, tingling, redness, painful blisters, and small ulcers.
In initial episodes, fever, malaise, body aches, and swollen lymph nodes near the affected area may also occur.
According to the Ministry of Health, the first activation tends to be more intense, while recurrences usually last less and present lower severity, although they still cause discomfort and impact daily life.
Moreover, the frequency of outbreaks varies from person to person.
Some people may have a single episode throughout their life, while others may face repeated reactivations, especially when triggering factors become more present.
The WHO emphasizes that recurrent outbreaks tend to be shorter than the initial episode, but they remain clinically and public health relevant because they maintain the risk of transmission.
Transmission of herpes and ways of contagion

Simple herpes spreads mainly through direct contact with saliva, skin, mucous membranes, secretions, or active lesions.
In the case of HSV-1, transmission usually occurs through oral contact, including kissing or sharing objects that have come into contact with saliva.
On the other hand, HSV-2 is more associated with sexual relations, even when there are no visible sores, because the virus can be transmitted during asymptomatic phases.
This point often causes confusion because many people associate contagion only with the appearance of blisters.
However, the WHO states that the risk is higher when there are active lesions, but transmission can also occur when the skin appears normal.
Therefore, controlling the infection depends not only on avoiding contact with visible sores but also on consistent preventive measures in daily and sexual life.
In genital herpes, this care becomes even more important because the infection is related to other vulnerabilities.
The World Health Organization points out that HSV-2 increases the risk of acquiring HIV by approximately three times.
The situation also requires attention in pregnant women, as, although rare, transmission to the baby during childbirth can cause neonatal herpes, an uncommon but potentially serious condition.
Treatment of herpes controls symptoms but does not eliminate the virus
There is no definitive cure for simple herpes, but there is treatment to shorten the duration of outbreaks, relieve pain, and reduce the frequency of recurrences.
The most commonly used antivirals include acyclovir, valacyclovir, and famciclovir, as directed by a physician.
According to the WHO and clinical reference manuals, these medications are most effective when started early, especially in the first hours or days of the outbreak.
In cases of frequent or very painful recurrences, the doctor may recommend suppressive therapy, with continuous use at a lower dose to decrease new episodes and reduce the chance of transmission.
However, the treatment does not remove the virus from the body.
It acts in clinical control, which reinforces the need for individualized follow-up, especially in people with immunosuppression, pregnant women, or patients with extensive symptoms.
Although most cases do not progress to severe forms, the impact should not be minimized.
Repeated lesions can affect eating, sleep, intimate relationships, and emotional well-being.
In immunocompromised individuals, herpes can become more severe and require quicker medical attention.
Ocular cases, for example, require specific care because there is a risk of significant complications when the infection reaches sensitive structures.
Prevention of herpes depends on information and routine
Prevention involves simple but continuous actions.
Avoiding kissing and intimate contact during outbreaks, not sharing objects that have touched saliva, using condoms correctly, and seeking medical evaluation in the face of recurring sores are central measures.
In oral herpes triggered by the sun, the WHO also recommends reducing intense exposure and adopting appropriate protection, as radiation can act as a trigger for new lesions.
It also helps to recognize early signs, such as burning, itching, and tingling, because this period precedes the appearance of blisters in many patients.
Identifying this pattern allows seeking guidance before the worsening of lesions and reducing the exposure of others to the virus.
At the same time, maintaining general health care, with stress control and attention to diseases that weaken immunity, can help reduce reactivations, although it does not completely prevent new episodes.
Finally, the advancement of knowledge about herpes has reinforced two essential points.
The first is that it is a very common infection, often silent and surrounded by misinformation.
The second is that correct diagnosis and treatment help control symptoms, reduce the risk of transmission, and prevent complications in more vulnerable groups, even without eliminating the virus from the body.

 Portuguese
Portuguese  English
English  Spanish
Spanish 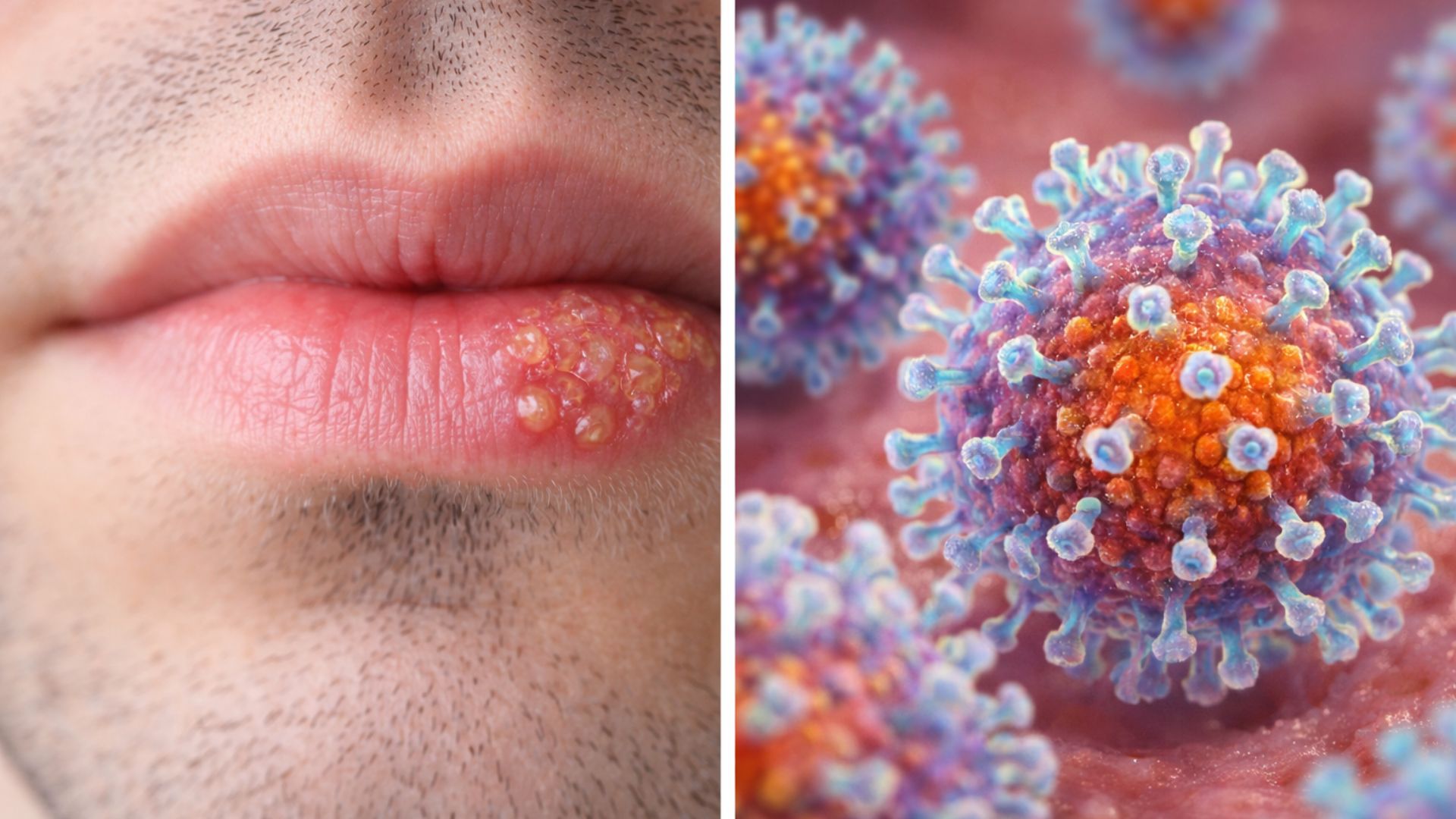





Seja o primeiro a reagir!